
I really like the UCSD Medical Campus on Campus Point Drive in La Jolla, California. It makes seeing my oncologist just a little more palatable. It’s open, airy, and refreshing compared to some other campuses that I’ve set foot on. Today was my fifth appointment with Doctor Stewart. The last time he laid out some potential therapies to treat my prostate cancer. This time I expected some more concrete plans. My wife, Jodie, waited with me in a small familiar exam room. Doctor Stewart was running behind schedule. Living with cancer has made me realize that “late” is subjective. He very well could be comforting another cancer patient in an exam room next door. Thirty minutes later he walked in, right on time.
One thing I like about my oncologist, and UCSD in general, is that a team of doctors work on your case. I’ve mentioned it in prior posts, but UCSD has a standing “Tumor Board” where all of the oncologists meet to discuss the cases for the week. It’s incredibly reassuring. Last week, the Tumor Board discussed my case and refined my treatment plan.
Continue Hormone Therapy
The first decision was to continue with the 2 years of hormone therapy. I wasn’t too surprised as after two months my PSA, or Prostate Specific Antigen level was now within the normal range. I can almost picture hundreds of thousands of emaciated prostate cancer cells, cinching their belts, sitting on their haunches, starving in a dry, barren wasteland. Testosterone? Fresh out, sorry.
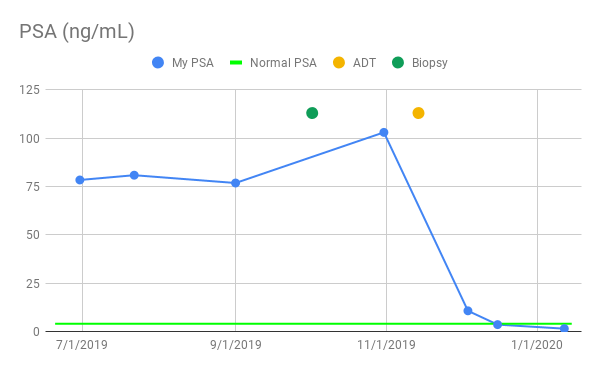
I created a chart for my PSA level and will start including it at the bottom of future posts. Keep in mind that PSA measures inflammation, and by extension, indicates cancer. However, after talking to Dr. Stewart, I realized that it doesn’t always measure how much cancer. Dr. Stewart told me that once prostate cancer metastasizes the scale diverges. As an example, he described one patient of his with bad metastasis to the bones who only had a PSA of 7.0. As far as my prior scans indicate, my cancer hasn’t metastasized in such a way, but my PSA was much higher at 103.
Side Effects
To menopausal women everywhere : I feel for you. I haven’t caved in and started fanning myself in public out of pride, but I have been tempted. The hot flashes, particularly at night, are bad. However, in a weird twist, I haven’t slept so soundly or have had such vivid dreams in years. Typically I wake up about four times a night in a sweat, stumble to the bathroom to drain my angry prostate, collapse into bed, and immediately fall back into a deep slumber to catch the latest of what’s playing on “Scott’s Twilight Cinema”. It’s bizarre and Dr. Stewart was more than a little concerned that I wasn’t getting enough sleep. When he asked if I wanted him to prescribe anything I just smiled back and shook my head “no”. I can only assume that my convenient narcolepsy is a result of sheer exhaustion from the hormone therapy as well as a result of my bedtime ritual of yoga, meditation, and prayer.
It’s not all “good” though, hormone therapy will totally mess with your emotions.
Now, I find myself crying for no reason, anywhere, anytime. I’ve never been the stoic emotionless type, but it’s a little ridiculous. To my friends and family, if you ever catch me with tears in my eyes, rest assured I’m likely having a medically induced man-o-pausal melodramatic moment.
And your libido …
Hormone therapy will destroy anything resembling libido. And, ( cough, cough ) it might even cause shrinkage. Now, I don’t make a habit of cupping my balls, but I’m pretty sure that they don’t hang so low or swing to and fro like they used to. Fortunately, I have read that this “condition” is temporary and is a direct result of the hormone therapy. In the meantime, I’ll just have a little extra real estate in my underwear.
And your liver …
Hormone therapy, particularly Zytiga, also messes up your liver function. During the first few weeks of being on the hormone therapy I saw my Bilirubin, ALT (SGPT) and Bi-Carbonate levels rise above normal. Bilirubin and ALT (SGPT ) are used to measure liver function. Bi-carbonate measures carbon dioxide in your blood. Jodie reminded me that when our oldest daughter Ashley was born, the doctor placed her under an artificial lamp to bring down her Bilirubin levels. She suggested that I try to get more sun and start taking walks throughout the day to bring mine down. Her advice seems to have worked because as of my last blood test my liver function has returned to normal.
And, it’s expensive …
Hormone therapy is outrageously expensive. Dr. Stewart initially started me on Firmagon, a monthly shot, to the tune of $3,837.23. The insurance company only covered $3,380.40 of this. I ended up paying $456.83 out-of-pocket. Since switching to Lupron, a shot that lasts three months, the cost has been reduced to $2,978.26. The insurance company covered $2,623.19, leaving me to pay $355.07 out-of-pocket. What a deal, right? Zytiga? Zytiga costs roughly $10,000 per month. I end up paying $10 per month after insurance, discounts, and financial aid.
Chemotherapy is off the table for now
The second decision made by the “Tumor Board” was to not do chemotherapy.
“For you, there is insufficient evidence that the benefits of chemotherapy would outweigh the risks.”, Dr. Stewart told me.
“My youngest daughter is going to be pissed”, I replied.
“How so?”
“She hates my beard. She was hoping chemotherapy would make it fall out.”, I replied.
Honestly, I was more than a little relieved. Chemotherapy works by poisoning the entire body with chemicals. The weaker cancer cells die. The stronger, non-cancer cells eventually recover. Chemotherapy affects all cells – including those belonging to the immune system. The immune system is responsible for fighting off colds, viruses, and most importantly, cancer. As I have spent the last few months attempting to cleanse and strengthen my body to fight my cancer, poisoning it just didn’t seem right. At least not at this point in my treatment. For now that particular arrow will remain in the quiver.
Surgery has been fast tracked
At the end of the month I have a consultation with Dr. Christopher Kane to discuss a radical prostatectomy, or the removal of my prostate.
I’m ready.
Three months ago when Scripps suggested it to me I wasn’t. Now I am. In fact, during my appointment, when Dr.Stewart told me that he wanted to discuss options for the next steps in my treatment, I interrupted him.
“Surgery”, I blurted out. “Even if we don’t get all of the cancer out, it will make me feel better knowing that the biggest source of it is no longer in me.”
“Is that what you would have chosen?”, I asked.
“Yes, if it were me I would choose surgery, too”, he replied.
Re-staging the Cancer
Before surgery Dr. Stewart wants to re-stage my cancer. When I asked why, he told me that cancer is re-staged to determine how it has responded to treatment or, to determine how much it has metastasized. Within the next few weeks I’m to undergo yet another CT Scan of my abdomen, chest, and pelvic region as well as another MRI of my prostate. The scans will act as a “map” for the surgeon during surgery. They might also show “scarring”, or places on my bones and tissue where the cancer has receded from as a result of the hormone therapy.
This will be my 3rd MRI and 3rd CT Scan in less than six months. I really need to ask if they have a rewards program.
Coffee enemas and other alternatives
Abruptly, Dr. Stewart turned to Jodie and asked, “So, what are you not letting him eat now?”
Ouch. I must have told him about the Thanksgiving Tofurkey.
I quickly butted in.
“The thing is, doctor, we’ve read a lot of articles on how a plant-based diet can be a good complementary treatment for cancer.”, I replied.
“Look, I just want to make sure that you’re not making yourself miserable. You should eat whatever makes you happy. There’s not a lot of evidence that a plant-based diet helps…”, he said.
I quickly glanced at Jodie, knowing that she was thinking exactly what I was thinking.
“We’ve both read a lot of books and studies that say that it does help. I’ve even read that cancer hates ginger and have started adding it to my tea.”, I said.
Doctor Stewart smiled.
“I add ginger to my tea, too…”. He started.
“…and you don’t have cancer!”, I joked.
“…the thing is, if you conduct a study enough times, chances are you’ll eventually get the results that you are looking for.”, he said, adding, “We’ve had at least a couple of patients that have refused treatments. One of them ended up at a clinic in Mexico getting coffee enemas.”
“Doctor Stewart”, I replied, “I told you from day one that I would do whatever you recommend. I realize that it is my best chance at being cured. However, Jodie and I are having a lot of fun with our plant-based diet. It’s delicious and I’m fortunate to have a wife that is a really good cook.”
“Okay, sounds good Just tell me if you start taking Saint John’s Wort or something crazy…”, he said.
Another DNA Test
Before we parted ways, Dr. Stewart brought up the results from my DNA testing.
“I don’t trust the results and want to send in another sample of your blood.”, he said.
Looking down at the bandage wrapped around my right arm I replied, “I had a blood draw this morning but I still have my left arm. Why don’t you trust the results? What are you looking for?”, I asked.
“Your last blood draw didn’t show any mutations and, given your family history and that the lab that we used took way too long with the results, I want to make sure that they are accurate.”, he said, “It will probably cost another $100.”
Sigh. What’s another hundred bucks.
To put it in perspective the grand total billed to our insurance company for my cancer treatment for 2019 was $75,857.70, and that does not even include the cost of medications. Shocking, right?
After shaking hands and parting ways I walked over to Moore’s Cancer Society to have a small vial filled with my blood. As I sat in the waiting room I couldn’t help but notice another lady my age, bald, wrapped in warm towels, slumped in a chair. I wanted to go over and talk to her, to compare war stories, to comfort her, but before I could muster the courage I was called in to have my blood drawn. When I was done, she was gone.
Having a Personal Chef Helps
I think what Doctor Stewart didn’t realize is that I have an excellent personal chef. There was definitely a learning curve. For the first few weeks of my transition to a plant-based diet I thought I’d be doomed to salads for the rest of my life. Fortunately, Jodie stepped up to the plate and I greatly appreciate it. It takes a lot of effort, too. She needs to shop for fresh produce at least twice a week. Now our freezer is mostly empty and our vegetable drawer is spilling out into the rest of the fridge.
Doctor Stewart is right. I shouldn’t put too much faith in my new diet, but it makes me feel better knowing that I am doing everything I can to beat my cancer.
Take care. Stay healthy. Live life.
-Scott
Previous : The plan, for now …
Next : I have a dream …
#prostatecancer #cancer #prostatitis #psa #prostate #urology #oncology #radicalprostatectomy #chemotherapy #hormonetherapy #surgery #lupron #leuprolide #firmagon #degarelix #docetaxel #drawnandcoded #iwillbeatthis

It really sounds like you are in good hands here Scott. I agree with doc about the plants. Keep going as long you enjoy it! I’ve had to curtail my plant-based ambitions as I’ve recently taken on the job of chef for the family. Like you said, its a lot of work to cook that way – especially when three of your diners just want chicken nuggets and are terrified of anything with a sauce! Stay strong my friend, you are doing awesome.
LikeLiked by 1 person
I know what you mean about kids. There’s only so many ways to disguise soy to make it look like something a kid will recognize. I guess I should emphasize a _low-sugar_ plant-based diet. The amount of sugar added to our processed foods scares me almost as much as the hormones and antibiotics that are pumped into our meat. Sugar has been long known to be cancers favorite snack. For me, I have to try everything I can. Good luck!
LikeLike
I am glad they aren’t going to poison millions of your healthy cells to (maybe) kill some bad ones. Sounds like the hormone therapy is working really well and the cleaner eating can’t hurt either as long as you are enjoying it thanks to your creative and talented wife/chef.
LikeLike
Great that your numbers are down! You are a terrific writer! You describe medical treatment so clearly and I love the humor that is included!
❤️Tia
LikeLiked by 1 person
I love this post so much and for many reasons…but mostly because you are one badass dude and your wife is kicking that Cancers ass one veggie at a time! Stay strong Scooty!
LikeLiked by 1 person
Keep on fighting, love the honesty in here. And you can always buy tighter underwear, or just stuff a sock down there like I do… 😉
LikeLiked by 1 person
Tried to send a comment 2 days ago but it didn’t show up!?????? Anyway, I usually carry tissue for colds, nose bleeds and for those emotional tears 😭. I knew you were always artistic but also love your clear informative writing with the great humor. Continue being positive!! Mom
LikeLiked by 1 person
I absolutely agree that the folks at the UCSD cancer center are great. A couple years ago when I went through something similar, I came to the conclusion that Dr. Kane was THE best urologist/surgeon in the San Diego area to do my radical prostatectomy. If you can get him, go for it! I would have had to wait a couple extra months to have him do my surgery, so he recommended Dr. Kader, who worked with and had been trained by him. I’m pretty sure everyone on the team there are top-notch.
You and your family are dealing with this SO well, and I admire your ability to stay positive, find humor, and especially to share so much of your experience and information with all of us.
Stay strong!
Carl
LikeLiked by 1 person
Thank, Carl. This is very reassuring. Take care 😉
LikeLike